
Trigeminal neuralgia (TN), also known as tic douloureux, is a pain disorder of the face affecting more than 15,000 people in the U.S. every year. The condition is characterized by sudden, intense pain coming from the trigeminal nerve, which spans the forehead, eye, cheek and jaw. While our trigeminal nerves are located on each side of the face, trigeminal neuralgia most commonly affects only one side.
TN is considered neuropathic pain and is generally caused by pinching of the nerve (neurovascular compression) from a nearby blood vessel.
Symptoms and Causes of TN
The pain of TN is often described as a sharp, electric shock-like pain that comes and goes and can be so severe that the affected person cannot eat or drink. The pain can last for a few seconds to minutes, can occur for days or weeks and can appear repeatedly during a day.
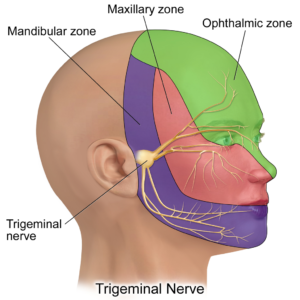
Symptoms of TN usually affect the three distinct branches of the trigeminal nerves, often referred to as V1, V2 or V3:
- The ophthalmic nerve (V1): The first branch controls sensations in a person’s eye, upper eyelid and forehead.
- The maxillary nerve (V2): The second branch controls sensations in the lower eyelid, cheek, nostril and upper lip.
- The mandibular nerve (V3): The third branch controls sensations in the jaw and lower lip.
TN is more common in women than men and occurs most often in people over age 50, although it can occur at any age. The disorder can also be caused by other conditions such as multiple sclerosis or as the result of oral surgery.
Treatment Options
There are several pain-relieving medications and even surgical procedures available to treat TN. About two-thirds of patients who suffer from TN successfully manage this condition with medications with carbamazepine (Tegretol®) being the first medication of choice.
Approximately one-third of patients are not successfully treated by medications or have side effects that are bothersome. In these cases, doctors recommend surgical treatment, which can include:
- Microvascular decompression (MVD) Surgery: Through a small opening in the back of the ear, the surgeon detaches the nerve from the offending blood vessel and separates them with a small sponge. The success rate to be pain free with MVD is approximately 85-90%.
- CyberKnife® radiotherapy: This is minimally-invasive radiation therapy that does not require open surgery. This is a good treatment option for patients with other diseases that make surgery risky or those who are adverse to surgery. Approximately one-third of patients are pain free without medications (face numbness is usually a sign of lasting pain freedom), one-third of patients are pain free with reduced medications and one-third of patients have reduced pain with the same medications.
- Rhizotomy (balloon/radiofrequency): This involves insertion of a needle through the cheek to crush or burn the trigeminal nerve and stop or reduce the pain. This modality is usually used after MVD or CK have been attempted or in patients with multiple sclerosis.
- Trigeminal nucleotractotomy: This is a surgical procedure to burn the center hub of face pain processing located in the brainstem. This procedure is carefully evaluated for patients with complex face pain syndromes.
The team at UofL Physicians – Neurosurgery includes fellowship-trained neurosurgeons who specialize in the treatment of TN. If you have questions or want to learn more about treatment options, contact our UofL Physicians – Neurosurgery team. Same-day/week appointments for urgent and emergent neurosurgical conditions and evaluation appointments are now available by calling 502-588-2160.









