 Your doctor tells you it’s time for a needed surgery—a hernia repair, perhaps, or gallbladder surgery, or a hysterectomy. You’re given the option of having open abdominal surgery vs. conventional straight stick laparoscopic surgery vs. robotic surgery (where the doctor uses a sophisticated da Vinci surgical system, or robot, to hold the scalpel). Should you take the robotic option?
Your doctor tells you it’s time for a needed surgery—a hernia repair, perhaps, or gallbladder surgery, or a hysterectomy. You’re given the option of having open abdominal surgery vs. conventional straight stick laparoscopic surgery vs. robotic surgery (where the doctor uses a sophisticated da Vinci surgical system, or robot, to hold the scalpel). Should you take the robotic option?
In most cases, yes. If your surgeon is comfortable and experienced with the technology, robotic surgery can allow him/her to perform the surgery (requiring only 8mm incisions) with enhanced 3-D imaging and magnification of tissue planes by 10x, along with finer dissecting ability and range of motion of wristed instruments that supersedes that of the human hand!
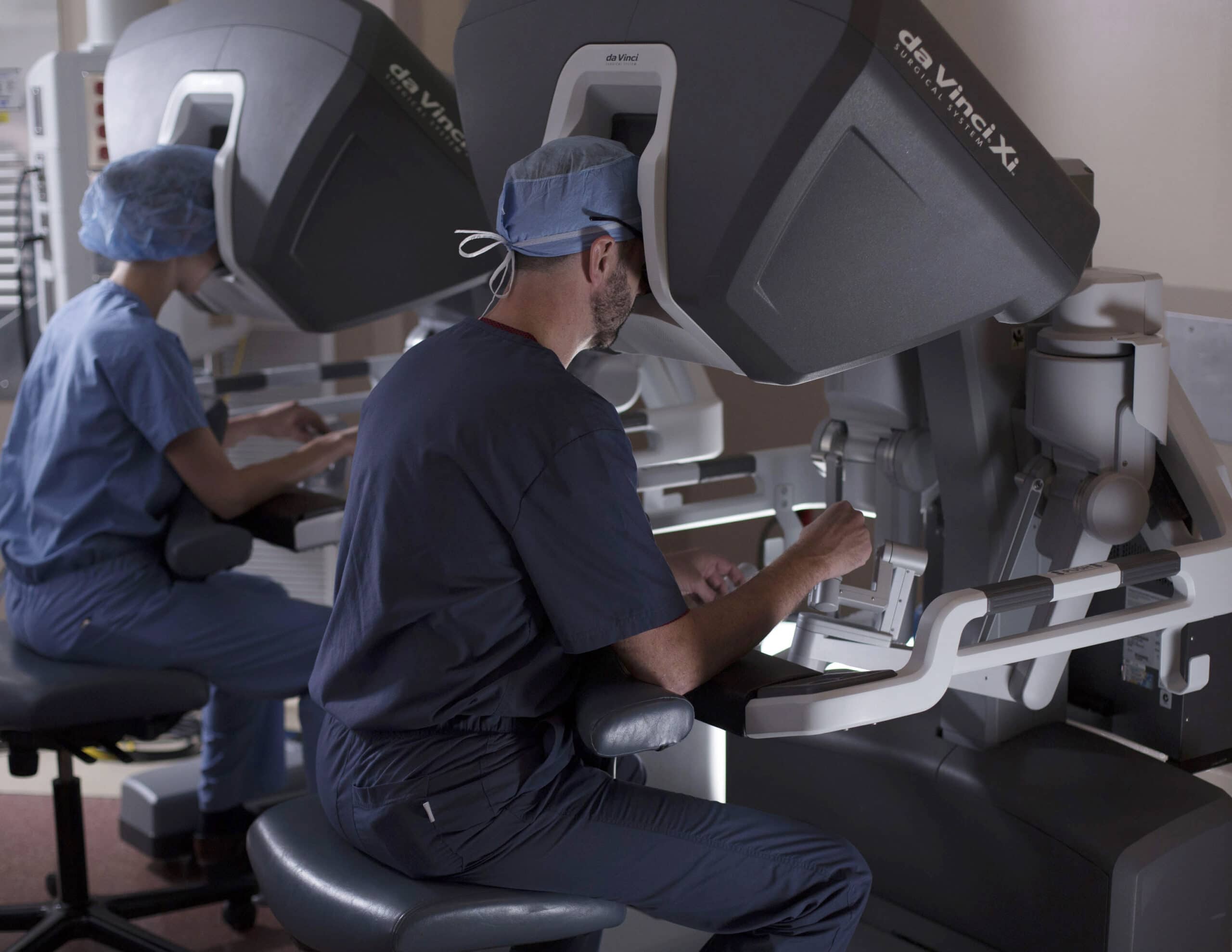
When a surgeon performs surgery robotically, he/she sits at a console within the surgical suite and controls the robot (which is attached to instruments inserted within the patient’s abdomen) with the use of his/her hands and feet using hand controllers and pedals. The robotic camera system projects a 3D image of the surgical field with 10x magnification to the console at which the surgeon is sitting. This enhanced imaging is critically important, since the surgeon is trying to work around healthy tissue and avoid injury to other organs, blood vessels and nerves. The robotic surgery system allows surgeons to see to a near microscopic level, eliminating guesswork. The robot can also rotate a full 360 degrees, offering an added degree of agility to the surgery, which allows for more surgeries to be completed minimally invasively instead of through a larger abdominal incision. All of these features of the robot correct for and bypass the limitations of conventional straight-stick laparoscopy as well.
So, what does this mean to you, the patient? Robotic surgery strives to provide you many surgical advantages over other approaches and quickens your recovery. In our practice here at UofL Health, we know that patients who undergo robotic surgeries see at least five main benefits of robotic surgery compared to other approaches. These include:
- Smaller incisions. Surgeons performing open surgery often must create larger incisions for access and appropriate exposure. However, with robotic surgery, 8mm incisions are all that are required to place ports within the abdominal wall. These ports allow access for robotic instruments to thread through and sync with the robot. Smaller incisions mean decreased risk of post-operative hernia formation and shortened healing time.
- Decreased post-operative pain. Robotic surgery affords less wear and tear on the abdominal wall given the smaller incisions and, thus, often results in significantly reduced post-operative pain. Some patients go home and never have to take any pain medication! Many others are well controlled post-operatively with ibuprofen and acetaminophen alone, avoiding narcotic use altogether.
- Decreased risk of infection and blood loss. Smaller incisions as well as the enhanced ability to perform finer surgical dissection allow for avoidance of significant blood loss during the procedure. Infection risk is also reduced, and this is particularly important in patients, who already have a number of other medical conditions to manage.
- Decreased length of stay in the hospital. Robotic surgery has seen a dramatic reduction in time required for post-operative recovery within the hospital. This is due in large part to better pain control, early return of bowel function, and faster healing. Getting patients home to their own beds safely is priority!
- Reduced abdominal wall scarring. Smaller incisions mean smaller, thinner scars, which can result in cosmetically-pleasing outcomes for patients.
To put it plainly, robotics has taken surgery to the next level. In my practice, we have enthusiastically embraced the technology and everything it does to improve patient care.
If you are being considered for surgery, don’t be afraid to ask whether or not you are a candidate for robotic surgery. UofL Health surgeons at UofL Health – UofL Hospital were the first in Kentucky to use the da Vinci system to perform a wide variety of operations, including colorectal surgeries, neobladder and Indiana pouch urinary diversions, and transoral procedures. Today, UofL Hospital is home to two da Vinci Xi systems, the most technically advanced robotic system on the market, and over 5,500 surgeries have been completed utilizing the da Vinci systems. Meanwhile, our cardiovascular and thoracic surgeons, in particular, have also begun utilizing the da Vinci Xi robotic system recently installed at UofL Health – Jewish Hospital. A true testament of the commitment of UofL Health to Jewish Hospital, this latest addition da Vinci Xi allows UofL Health to offer even more robotic surgeries with wider applications to our patients.









