How do I prepare for my surgery/procedure?
Thank you for choosing UofL Health – Jewish Hospital and UofL Health – UofL Hospital for your surgery/procedure. We take great pride in making your experience as comfortable as possible.
Days Before Surgery/Procedure
A registered nurse will contact you by telephone several days prior to your surgery/procedure. The nurse will:
- Provide you with information on your surgery/procedure
- Ask for your medical history
- Answer any questions you may have
- Based on your medical history and/or procedure, you may also be asked to make an appointment for a preoperative anesthesia clinic visit.
- You may receive a call to verify your insurance and notify you of any co-pay required on the day of the surgery/procedure.
Day of Surgery/Procedure
- Please do not wear jewelry, hair pins or makeup and remove all piercings.
- Leave all unnecessary valuables at home.
- Wear loose fitting, comfortable clothing that will be easy to put back on after surgery/procedure.
- Please avoid using any alcohol-based products in your hair, including gels, hairspray or mousse products.
- Take your morning medications as instructed by your provider or nurse.
- Follow specific fasting instructions.
- If you become ill the morning of surgery/
procedure, are running late or are unable to make it to your surgery/procedure, please notify your doctor right away.
Plan Ahead
- Arrange for transportation to and from the hospital. You may NOT drive yourself home or take public transportation after your surgery/procedure without a responsible designated person. Please make arrangements before arriving at the hospital.
- If you are discharged the day of your surgery/procedure, it is best to have someone with you for at least the first 24 hours after general anesthesia.
Medications
Some medications may need to be stopped prior to surgery/procedure. Recommendations will vary based on your medical history and the surgery/procedure you are having.
- Blood thinning medications (Aspirin, Plavix®, Coumadin®, Pletal®, Xaralto®, Eliquis®) may need to be stopped several days before surgery/procedure. It is important that you discuss with your surgeon and/or provider the optimum timing for stopping these medications.
- Herbal medications/supplements and prescription diet medications (Phentermine) should be stopped one week prior to surgery/procedure.
- Aleve® and Naproxen should generally be discontinued at least three days before surgery/procedure. Ibuprofen should be stopped 24 hours prior to surgery/procedure. Acetaminophen can be taken up to the day of surgery/procedure.
- If you are taking certain rheumatologic medications (Etanercept, Rituximab®), please discuss the timing of discontinuation with your rheumatologist.
- If you have insulin dependent diabetes, refer to your endocrinologist or primary care provider for day of surgery/procedure insulin dosing.
When to Stop Eating and Drinking
PLEASE NOTE: If you do not follow preoperative fasting instructions as recommended, your surgery/procedure may be delayed or canceled.
- “Fasting or NPO” means not eating or drinking for a certain period of time. Fasting is necessary to prevent food or liquids in your stomach from entering your lungs (aspiration) when you are given anesthetic medication for your surgery/procedure.
- Avoid chewing tobacco for six hours or non-tobacco products including chewing gum for at least two hours prior to the scheduled surgery/procedure.
- If you are instructed to drink a bowel preparation (ex. Golytely or Magnesium Citrate) prior to your surgery/procedure, you may only drink clear liquids from the start of your prep up until the recommended stopping time.
- If you were instructed to take medication the morning of surgery/procedure, please take it at least two hours prior to your scheduled surgery/procedure time with clear liquids.
- Patients with medical conditions that may affect stomach emptying (uncontrolled gastroesophageal reflux, hiatal hernia or gastroparesis) should not eat eight hours prior to your surgery/procedure with the exception of clear liquids as recommended.
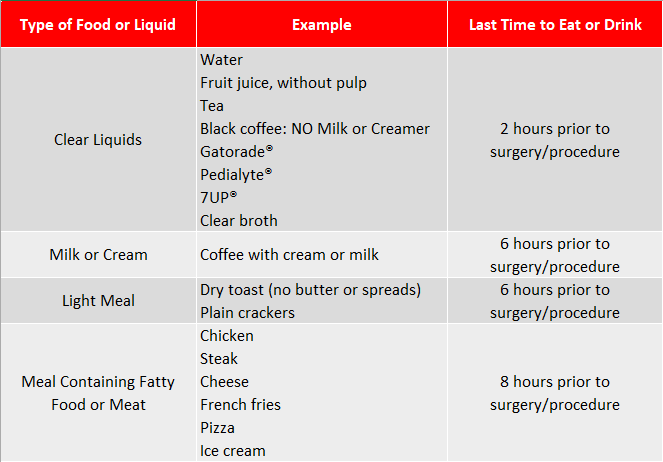
For children and adults without diseases or conditions that might affect stomach emptying, please adhere to the guidelines in this table.
Preventing Surgical Site Infections
- Skin is a natural barrier to infection. Although many precautions are in place to prevent infection, any break in the skin, such as a surgical incision, can lead to an infection. Although infections are rate, they can make recovery from surgery/procedure more difficult because they can cause additional illness, stress and cost. It is important to follow all prevention recommendations.
- Bathe or shower with antimicrobial soap (Dial®, Safeguard®, Lever2000®) or chlorhexidine wash the night before and morning of surgery/procedure as directed.
- Sleep in clean sheets and pajamas the night before surgery/procedure.
- Do not shave near where you will have surgery/procedure. Shaving with a razor can irritate your skin and make it easier to develop an infection.
- Part of preventing surgical site infections is keeping your body temperature warm. Please wear warm clothes, especially during the winter months. To help keep your temperature normal. In the preoperative room, we will begin to actively warm you. We will continue this during and after your surgery/procedure.
- Wash hands with soap and water or an alcohol-based hand rub.
What to expect on the day of surgery or procedure?
Preoperative Room
- Once settled in your preoperative room, you will be asked to put on a hospital gown. Depending on the type of surgical procedure you are having, you may be asked to cleanse your skin with an antimicrobial agent.
- Your nurse will start an IV and review medications and medical history.
- Your surgeon, anesthesiologist, nurse anesthetist and operating room nurse will also visit with you, reviewing medications and medical history. They will answer any questions you may have.
Operating/Procedure Room
- Once in the operating room, the team will call a “time out” to perform additional checks to ensure your safety. Your skin will be cleansed with an antimicrobial agent. All body areas will be draped except the part that will be operated on. Depending on the length and complexity of your surgery/procedure, a number of other team members will be present.
- During your procedure, your health care providers will keep you safe and continuously monitor you.
Recovery Room
- After surgery/procedure, you will then be taken to the Post Anesthesia Care Unit (PACU) or your recovery room.
Recovery Phase I
- Your nurse will monitor your vital signs and provide medication for your pain and/or nausea.
- Average recovery time is one to two hours.
- Visitors are not allowed during this recovery time.
- If you are staying overnight in the hospital, you will be moved directly from the recovery room to the room you will be staying in. Your family will be notified of your inpatient room at this time and may meet you there. In the event the hospital is full, you will remain in the PACU until a room is available.

Recovery Phase II
- If you are going home the same day, you will be moved to a post-recovery room where you can see your family and/or friends.
- At this time, you are generally awake; you may start drinking small amounts of fluid and can go to the restroom with assistance.
- When discharge criteria have been met, you will be given post-operative instructions and will be transported by wheelchair out of the hospital.
Pain Management
Your comfort after surgery/procedure is a priority and of great importance to us.
We will often use a variety of ways to help make you comfortable-including oral medications, intravenous medications, injection of local anesthetic, peripheral nerve blocks and relaxation techniques.
Pain is different for everyone. We will be assessing your comfort level from the time of admission until you receive your post-operative call at home. During your stay at the hospital, you will be asked to rate your pain using a numerical scale (0 to 10) or the “Faces Pain Scale.”
After Discharge Phone Call
UofL Health - UofL Hospital is committed to providing high-quality health care. A few days after surgery/procedure, you will receive a survey and phone call from a member of our hospital staff to discuss your stay and see how you are feeling. We encourage you to take this opportunity to provide us with comments and suggestions regarding our services. Thank you for trusting us with your health care needs.
Day of Surgery Packing Checklist
❑ Insurance card, identification card and your co-pay
❑ Copy of advanced directive or living will, if not currently on file
❑ Storage containers for eyeglasses, contacts, dentures and hearing aids
❑ An up-to-date medication list
❑ Cane, crutches or walker, if needed
❑ C-Pap or Bi-Pap machine, if needed
❑ Small bag of personal items if staying overnight (robe, slippers, toothbrush, pajamas, undergarments)
❑ Portable oxygen for your trip to and from the hospital, if needed
❑ Rescue inhalers, if needed
Questions
If you have questions about preparing for your surgery, please call your provider’s office.



